12 Key Care Priorities During the Golden Hour of Prematurity
The first hour of life is a critical window in neonatal care. For preterm newborns—especially those with very low or extremely low birth weight (<1500 g / <1000 g)—early interventions play a decisive role in stabilization and in reducing the risk of complications.
This period, known as the Golden Hour, refers to a structured set of timely, coordinated, and evidence-based interventions designed to support the newborn’s transition to extrauterine life and improve both immediate and long-term outcomes.
Why the Golden Hour Matters
When applied consistently, Golden Hour protocols help improve clinical efficiency and patient outcomes. These interventions contribute to better temperature control at admission, faster transfer to the NICU, and earlier initiation of critical therapies.
Early stabilization also supports quicker surfactant administration, timely nutritional support, and efficient vascular access. Together, these measures help reduce the incidence of complications such as intraventricular hemorrhage, hypoglycemia, chronic lung disease, and retinopathy of prematurity.
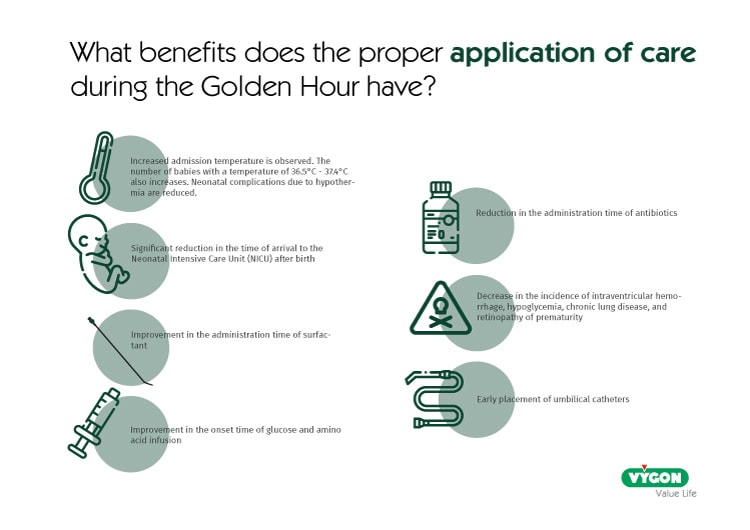
The 12 Essential Care Priorities
1. Prenatal Counseling and Team Preparation
Preparation begins before delivery. Close coordination between obstetric, neonatal, and nursing teams ensures readiness, proper equipment availability, and optimized workflow. Supporting and informing parents is equally essential during this stage.
2. Delayed Umbilical Cord Clamping
When clinically appropriate, delaying cord clamping by 30–60 seconds can support cardiovascular transition, improve pulmonary circulation, and reduce the need for transfusions and the risk of complications.
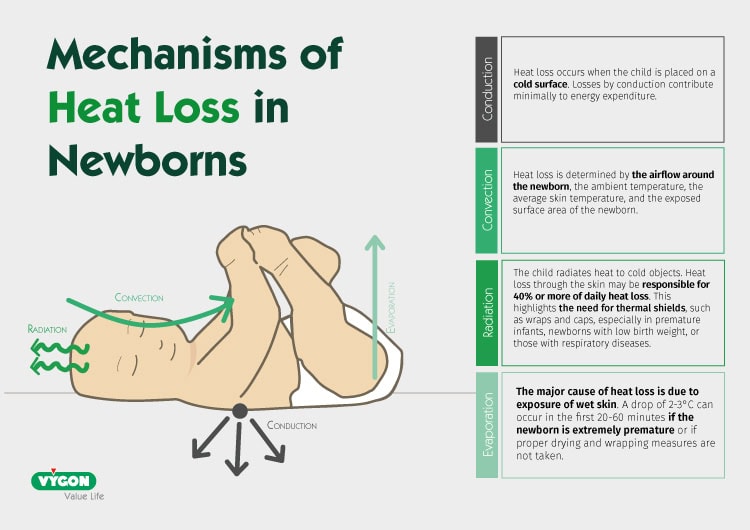
3. Prevention of Hypothermia
Preterm infants are highly vulnerable to heat loss. Maintaining thermal stability is critical, as even a small drop in temperature can significantly increase the risk of mortality and complications.
Strategies include controlling delivery room temperature, using thermal wraps, minimizing exposure, and applying additional heat sources such as radiant warmers and heated mattresses.
4. Safe Transport During the Golden Hour
Newborn stabilization must occur before transport. During transfer, maintaining body temperature and continuous monitoring of vital functions is essential to ensure safe transition to the NICU.
5. Respiratory Support
Preterm infants often require assistance initiating effective breathing. Non-invasive support such as CPAP is recommended when spontaneous breathing is present, while invasive ventilation may be required in more critical cases.
6. Surfactant Administration
Due to limited surfactant reserves, early administration is key in managing respiratory distress syndrome. Less invasive techniques are preferred when possible to reduce the need for mechanical ventilation.
7. Cardiovascular Support
Continuous monitoring of heart rate, blood pressure, and perfusion is essential. Early assessment allows timely intervention, particularly in cases requiring resuscitation.
8. Early Nutrition and Amino Acid Administration
Once placental supply stops, early nutritional support becomes critical. Initiating glucose and amino acid administration helps maintain metabolic stability.
9. Prevention of Sepsis
Strict adherence to aseptic techniques is essential, as preterm infants are highly vulnerable to infection. Infection prevention remains a key priority during all interventions.
10. Laboratory Studies
Key laboratory tests should be performed early to guide clinical decisions. These may include blood gases, glucose levels, cultures, and imaging when required.
11. Monitoring and Documentation
All vital signs, interventions, and timings should be accurately recorded. Detailed documentation supports evaluation of care effectiveness and ensures continuity of treatment.
12. Communication with the Family
Clear, compassionate communication with parents is essential throughout this critical period. Keeping families informed helps build trust and supports decision-making.
Conclusion
The Golden Hour represents a structured and evolving approach to neonatal care. By applying standardized protocols and ensuring strong multidisciplinary collaboration, healthcare teams can improve both immediate stabilization and long-term outcomes for preterm infants.
Consistency, education, and adherence to best practices remain key to maximizing the impact of Golden Hour interventions.

Support your Golden Hour protocols with reliable clinical solutions.
Discover products designed to enhance efficiency, safety, and patient outcomes.
Resource
This article was adapted from educational content originally published by Campus Vygon: “12 cares to be performed during the golden hour of prematurity.”
Original source: Campus Vygon, 2026.

